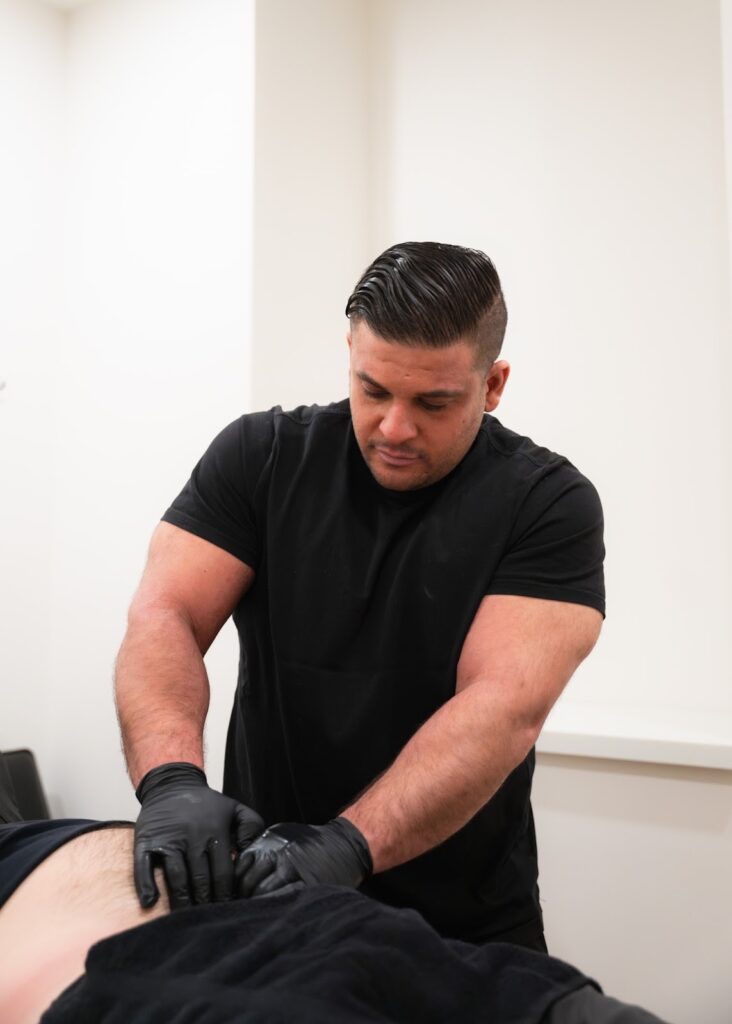
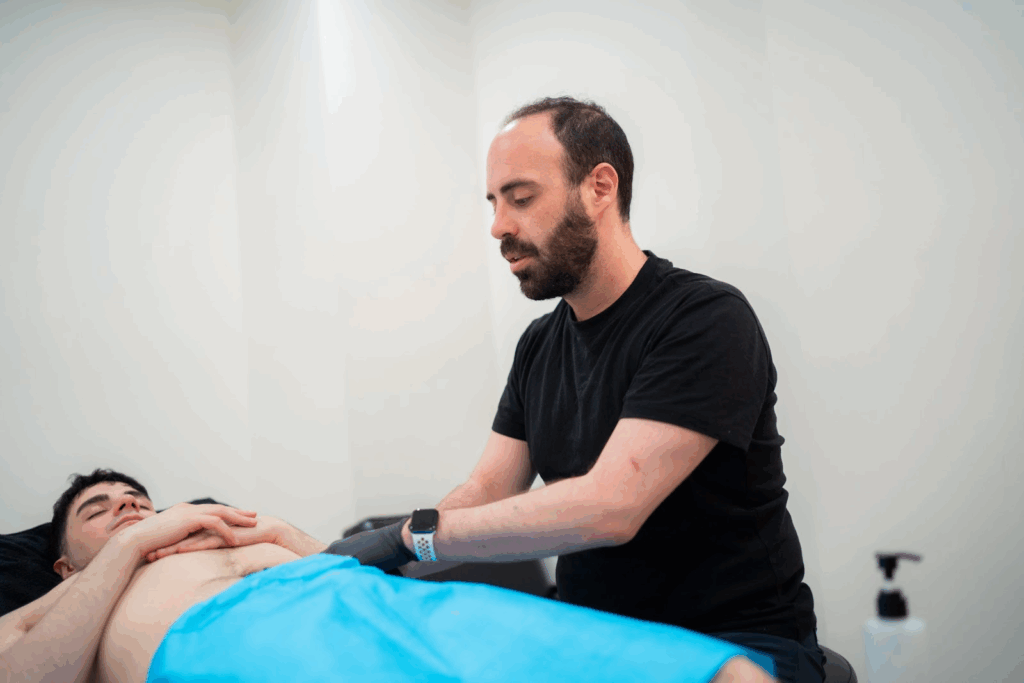
What Are Urinary Problems?
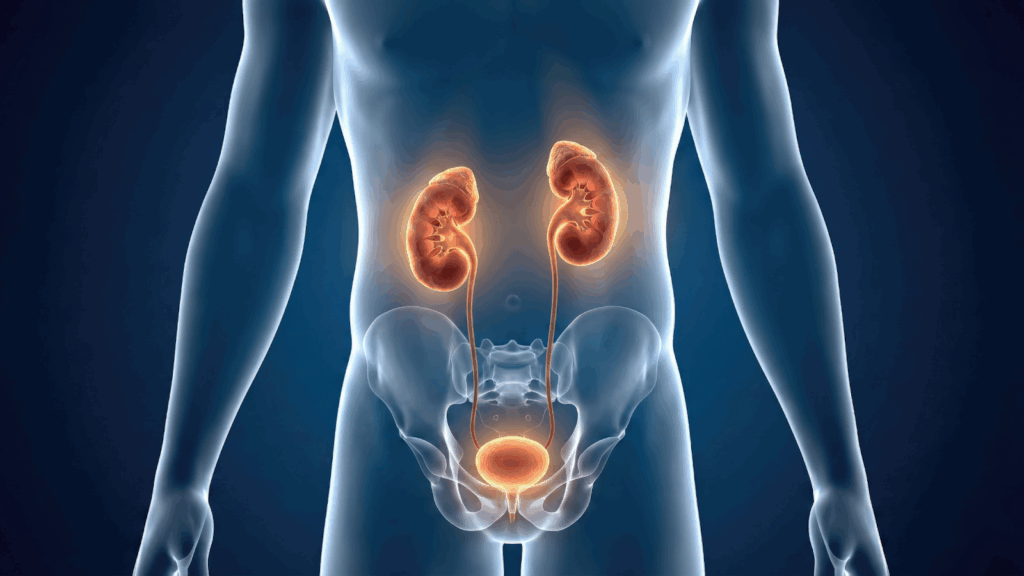
Urinary problems refer to symptoms that affect how often, how easily, or how comfortably you urinate. They can include urgency, leakage, pain, difficulty emptying the bladder, or frequent trips to the bathroom—and they affect people of all ages and genders.
While common, urinary issues are not something you have to “live with.” Most are treatable once the underlying cause is identified. In fact, most people with urinary problems can find significant relief with proper treatment.
Read about Managing Urinary Issues: Expert Tips from a Physical Therapist
Why Urinary Problems Happen
Urinary symptoms rarely have just one cause. They often result from a combination of bladder, pelvic floor, prostate, nervous system, and lifestyle factors.
Certain medications and medicines, such as diuretics and decongestants, can contribute to urinary problems by increasing the need to urinate or affecting bladder health. Some medicines can disrupt the normal process of storing and passing urine or increase the amount of urine you produce. It is important to consult a doctor before discontinuing any medication that may affect urination, as professional guidance is essential in managing these conditions.
According to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), over 25 million adults in the U.S. experience urinary incontinence, yet many never seek care.
Urinary Problems Symptoms
Urinary problems can range from mild inconvenience to life-disrupting conditions. Some develop gradually, while others appear suddenly.
Common signs include:
- Needing to urinate often
- Difficulty starting or finishing urination
- Leakage or loss of bladder control
- Pain or burning with urination
- Feeling like the bladder never fully empties
- Blood in urine
- Strong urge to urinate
- Urge to urinate
Blood in the urine can be a sign of a serious illness such as kidney or bladder stones, an infection, or bladder or kidney cancer.
Some people may have difficulty passing urine or may feel a strong urge to pass urine suddenly.
Symptoms can also include pain during urination (dysuria), waking frequently at night (nocturia), and lower abdominal pain.
These symptoms can point to issues in the urinary tract, bladder muscles, pelvic floor, or prostate.
Urinary Tract Infections
Urinary tract infections (UTIs) are one of the most common causes of urinary problems, especially in women.
The best thing to do for a urinary tract infection is to see a healthcare provider.
Typical UTI symptoms include:
- Painful urination
- Frequent urination with small amounts
- Urgency
- Cloudy or strong-smelling urine
Signs of urinary tract infections also include burning sensation, frequency, urgency, and blood in the urine. You need antibiotics to treat a UTI, and healthcare providers commonly prescribe antibiotics for this purpose. It’s very important to follow the directions for taking antibiotics and to take the full course, even if symptoms go away. Most people feel better within a few days after starting antibiotics. Minor urinary tract infections can sometimes get better on their own, but most need antibiotics to go away. Medication options for urinary issues include antibiotics for UTIs and medications to relax the bladder or prostate muscles. If you get UTIs often, a healthcare provider may give you low-dose antibiotics for a short time to prevent the infection from coming back. Cranberry extract supplements may decrease your chances of getting a UTI.
While antibiotics treat the infection, recurrent UTIs and frequent or chronic bladder infections may be linked to pelvic floor dysfunction or incomplete bladder emptying—issues that pelvic floor physical therapy can address. Recurrent or chronic bladder infections may also indicate an underlying bladder issue.
Frequent Urination
Frequent urination means urinating more often than usual, including waking up at night (nocturia).
Possible causes:
- Overactive bladder
- Pelvic floor muscle tension
- UTIs
- Prostate enlargement
- Excess caffeine or fluid intake
- Certain medications, such as diuretics and decongestants
It’s not always a bladder problem—sometimes the pelvic floor is too tight to allow normal storage and release.
Painful Urination
Painful urination (dysuria) may feel like burning, pressure, or sharp pain.
Common causes include:
- UTIs
- Bladder inflammation
- Pelvic floor muscle spasm
- Nerve irritation
If tests repeatedly come back “normal,” pelvic floor dysfunction is often overlooked—but highly treatable.
Urinary Incontinence
Urinary incontinence is the involuntary leakage of urine. It affects millions of people but is not a normal part of aging.
There are several types, including stress and urge incontinence.
Stress Incontinence
Stress incontinence occurs when pressure is placed on the bladder.
Triggers include:
- Coughing or sneezing
- Laughing
- Exercise
- Lifting
It’s often linked to pelvic floor muscle weakness or poor coordination, especially after pregnancy or surgery.
Urge Incontinence
Urge incontinence involves a sudden, intense need to urinate followed by leakage.
It’s commonly associated with:
- Overactive bladder
- Pelvic floor muscle tension
- Nervous system sensitivity
Contrary to popular belief, strengthening alone is not always the solution—learning to relax the pelvic floor is often key.
Bladder Control
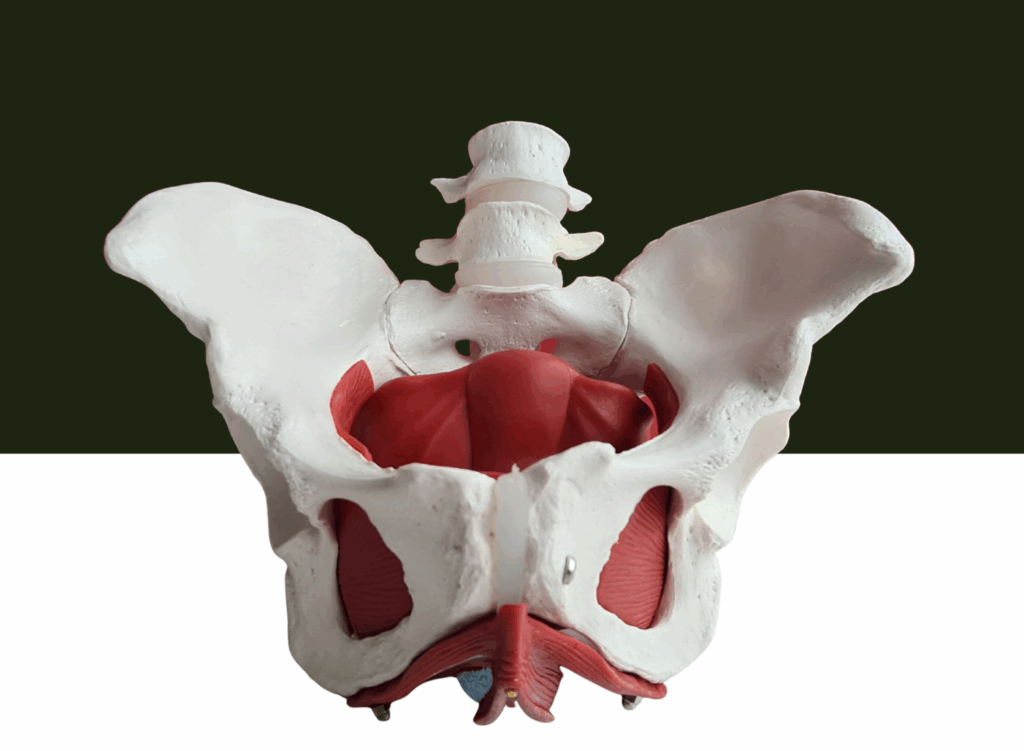
Healthy bladder control depends on proper communication between:
- The bladder
- Pelvic floor muscles
- Nervous system
The detrusor muscles contract to allow urine to be released through the toilet during the process of emptying the bladder.
When muscles are too tight or poorly coordinated, bladder signals become exaggerated, leading to urgency and leakage.
Difficulty Emptying
Difficulty emptying the bladder may feel like:
- A weak urine stream
- Stopping and starting
- Feeling “not done” after urinating
This is often related to:
- Pelvic floor muscle tension
- Poor relaxation during voiding
- Prostate issues in men
- Obstruction (such as bladder stones, ureteral obstruction, or an enlarged prostate)
Overflow incontinence occurs when the bladder cannot empty completely due to a blockage or obstruction.
Acute urinary retention is characterized by an inability to urinate, sometimes accompanied by fever or severe pain.
Incomplete emptying can increase UTI risk and bladder irritation.
Prostate Problems
In men, prostate gland problems are a common contributor to urinary issues.
Surgery or radiation for prostate cancer may lead to nerve damage, bladder spasms, or stress incontinence.
Enlarged Prostate
An enlarged prostate (BPH) can cause:
- Weak urine stream
- Hesitancy
- Dribbling
- Frequent urination
However, research shows pelvic floor muscle dysfunction often coexists with BPH, meaning symptoms may persist even after medication unless muscle tension is addressed.
Risk Factors for Urinary Issues
Urinary issues, such as urinary incontinence and urinary tract infections, can affect anyone, but certain factors increase your risk. Age is a significant factor—older adults are more likely to experience problems like weak urine stream, frequent urination, and difficulty emptying the bladder. Gender also plays a role: women are more prone to stress incontinence due to changes in pelvic muscles, especially after childbirth or menopause.
Other important risk factors include obesity and chronic conditions like diabetes, which can impact the urinary tract and bladder function. A history of digestive and kidney diseases can also make urinary symptoms more likely. For men, an enlarged prostate—known as benign prostatic hyperplasia (BPH)—is a common cause of urinary difficulties, including trouble starting urination and incomplete bladder emptying.
By understanding these risk factors, you can take proactive steps to protect your urinary system and reduce the likelihood of developing incontinence or other urinary problems.
Diagnosis and Treatment Options
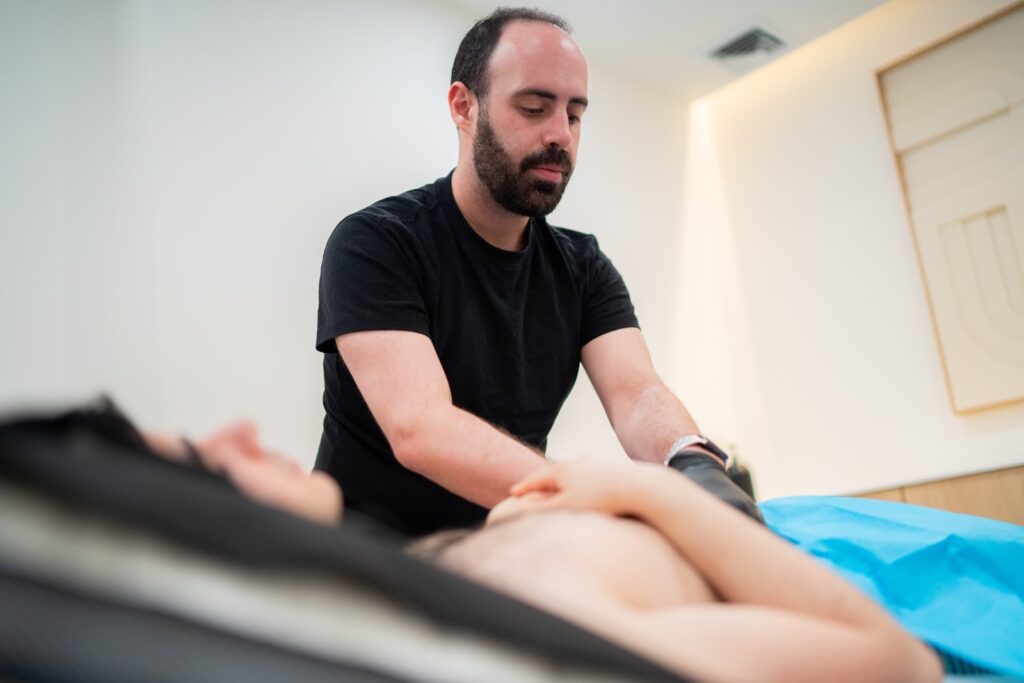
Getting to the root of urinary symptoms starts with a thorough medical history and physical examination. Your healthcare provider may ask about your symptoms, lifestyle, and any history of digestive or kidney diseases. Diagnostic tests, such as urinalysis or urine culture, help identify infections or other underlying issues in the urinary tract.
Treatment options depend on the specific cause. For urinary tract infections, antibiotics are usually prescribed to clear the infection. Stress incontinence often responds well to lifestyle changes, including pelvic floor exercises and weight management. In cases of enlarged prostate or urinary tract blockage, surgery may be recommended to restore normal urine flow. Managing chronic conditions like diabetes is also crucial for reducing urinary symptoms and preventing complications.
Consulting a healthcare professional ensures you receive the right diagnosis and treatment. Trusted organizations like the National Institute of Diabetes and Digestive and Kidney Diseases and the American College of Physicians offer up-to-date guidelines and resources to help you make informed decisions about your urinary health.
Preventing Urinary Problems
Prevention is key to maintaining a healthy urinary system. Simple lifestyle changes can make a big difference—stay well-hydrated, limit alcohol and caffeine, and practice good hygiene to reduce your risk of urinary tract infections. Regular physical activity and a balanced diet support overall health and help prevent issues like obesity and diabetes, which are linked to urinary problems.
Listening to your body is important: don’t delay urination when you feel the urge, and avoid holding urine for long periods. For men, maintaining a healthy weight and getting regular check-ups can help prevent prostate problems. Medical education and awareness are powerful tools—organizations like the Mayo Foundation provide reliable information on urinary health and prevention strategies.
By adopting these habits and staying informed, you can lower your risk of urinary tract infections, incontinence, and other urinary issues, supporting your health for years to come.
How Pelvic Floor Physical Therapy Helps Urinary Problems
Pelvic floor physical therapy is one of the most effective, evidence-based treatments for urinary dysfunction.

A pelvic floor therapist can help:
- Improve bladder control
- Reduce urgency and frequency
- Address leakage
- Retrain pelvic floor muscle coordination
- Reduce muscle tension that interferes with urination
According to the American Physical Therapy Association (APTA), pelvic floor physical therapy is a first-line treatment for many types of urinary incontinence.
When to Seek Help
You should seek professional care if:
- Urinary symptoms persist longer than a few weeks
- You experience pain, leakage, or difficulty emptying
- Symptoms interfere with daily life or sleep
Early care prevents long-term complications.
Why Choose Pelvis NYC?
Pelvis NYC specializes exclusively in pelvic floor physical therapy. Their clinicians have advanced training in treating complex urinary problems across all genders.
Patients benefit from:
- One-on-one expert care
- Evidence-based treatment plans
- A supportive, judgment-free environment
👉 Schedule a consultation with Pelvis NYC to address urinary problems at the root—not just mask symptoms.
Frequently Asked Questions (FAQ)
What causes urinary problems?
Urinary problems can result from bladder dysfunction, pelvic floor muscle issues, UTIs, prostate problems, nerve irritation, or lifestyle factors.
Are urinary problems normal with age?
They’re common, but not normal or inevitable—and they’re often treatable.
Can pelvic floor physical therapy help urinary symptoms?
Yes. It’s one of the most effective treatments for incontinence, urgency, and difficulty emptying.
Do Kegels help all urinary problems?
Not always. Tight pelvic floor muscles may need relaxation before strengthening.
When should I see a specialist?
If symptoms are persistent, painful, or affecting quality of life, seek care early.