To recover from chronic male pelvic pain, you must address the physical tension of the muscles and the protective “fight-or-flight” response of the nervous system. For many men, including Daniel, traditional surgery fails because it treats structural issues without retraining the hypertonic pelvic floor to relax. True healing occurs through specialized pelvic floor physical therapy that integrates nervous system regulation with manual muscle release.
The Silent Epidemic of Male Pelvic Pain

For years, Daniel lived with a secret that felt like a life sentence. At 18, following a traumatic experience, his body began to “guard” itself. What started as discomfort during bowel movements evolved into a decade-long cycle of chronic pain, substance use to numb the discomfort, and an overwhelming sense of isolation. Many individuals with chronic pelvic pain have a history of sexual or physical abuse, and comorbid posttraumatic stress disorder (PTSD) is common, which can exacerbate symptoms and complicate treatment.
Daniel’s story is not rare; it is simply rarely discussed. Chronic Pelvic Pain Syndrome (CPPS) affects approximately 2% to 10% of men worldwide. Chronic pelvic pain accounts for 2% to 16% of cases in men, and the overall prevalence among women ranges from about 4% to 16%. It rarely has a single source and is often categorized based on the affected system. Examples are gynecological, urinary, gastrointestinal, musculoskeletal, and nerve-related issues. Yet many are misdiagnosed with recurring prostatitis or told their issues are “all in their head.”
The “Broken” Narrative
When Daniel finally sought medical help, he was diagnosed with an anal fissure and hemorrhoids. He underwent a sphincterotomy, hoping surgery would be the “quick fix.” Instead, he encountered:
- Post-op complications: Including a week without a bowel movement.
- Secondary issues: Developing a painful fistula and hematomas.
- Psychological trauma: Undergoing painful cauterization and being told he may never have penetrative sex again.
- Emotional trauma: Emotional trauma, including the psychological impact of surgery and negative prognoses, can contribute to the persistence and complexity of chronic pelvic pain. Persistent pain after surgery is not uncommon; for example, approximately 28% of women experience persistent pelvic pain 3 months after an elective cesarean delivery, with 20% continuing to have persistent pain 6 months postoperatively.
This is the moment many men give up. When the “experts” tell you your body is permanently scarred or broken, the nervous system locks into a state of permanent high alert.
Diagnosing Chronic Pelvic Pain
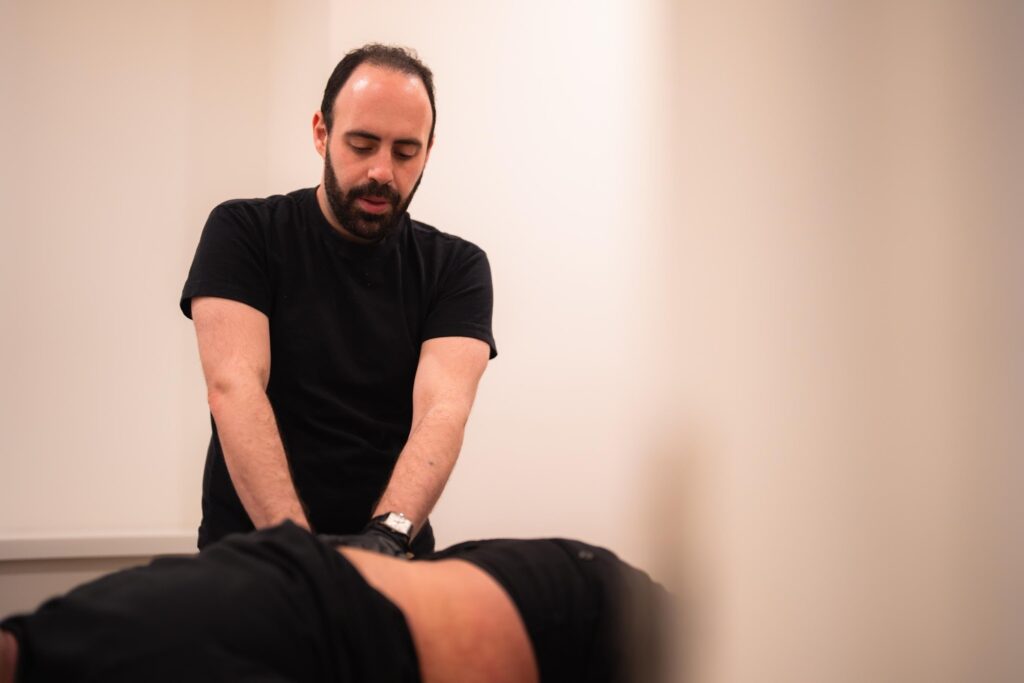
Diagnosing chronic pelvic pain is often a journey that requires patience, persistence, and a comprehensive approach. Because the pelvic region is home to a complex network of muscles, nerves, and organs, pinpointing the exact cause of pelvic pain can be challenging. The process typically begins with a detailed medical history, where your healthcare provider will ask about your symptoms, lifestyle, and any previous medical issues, such as irritable bowel syndrome or pelvic inflammatory disease.
A thorough physical examination is a crucial next step. During this exam, your provider will assess for tenderness, muscle tightness, or abnormalities in the pelvic organs. Depending on your symptoms, imaging tests like pelvic ultrasound or magnetic resonance imaging (MRI) may be recommended to get a clearer picture of what’s happening inside your body. These tools help rule out structural problems and identify potential sources of chronic pelvic pain.
Laboratory tests, such as blood work or urinalysis, may also be used to check for infections or other underlying conditions. Because chronic pelvic pain can be linked to a variety of issues—including irritable bowel syndrome, pelvic inflammatory disease, and even endometriosis—a multidisciplinary approach is often necessary. This means working with specialists in gynecology, urology, and gastroenterology to ensure that all possible causes are explored and addressed. Ultimately, a careful and thorough diagnostic process is the first step toward finding lasting relief.
What is a Hypertonic Pelvic Floor?
When Daniel finally found Pelvis NYC, the diagnosis wasn’t a structural “break,” but a functional one: a hypertonic pelvic floor.
A hypertonic pelvic floor occurs when the muscles surrounding the bladder, prostate, and rectum stay in a state of constant contraction. They “forget” how to relax.
This type of persistent pain can also be described as a functional somatic pain syndrome, a non-specific, centralized pain condition often linked to psychological or neurological factors. Chronic pelvic pain may develop due to central sensitization, where the nervous system becomes overly sensitive to pain stimuli, a process often exacerbated by comorbid anxiety and depression.
Why the Body Stays Tight
The human body is designed to protect itself. When we experience trauma—whether it’s a physical injury, a surgery, or sexual assault—the pelvic floor muscles often contract to shield the area. A history of physical abuse is a significant risk factor for developing chronic pelvic pain. Developing chronic pelvic pain can result from a combination of risk factors, including trauma, surgery, and psychological stress.
In Daniel’s case, the cycle looked like this:
- Trauma/Surgery: Initial pain triggers muscle guarding.
- Fear of Pain: Anticipating pain during a bowel movement causes the brain to send “danger” signals.
- Chronic Tension: The muscles stay tight 24/7 to “protect” the area.
- Nerve Irritation: Constant tension irritates local nerves, creating more pain.
Understanding Nonspecific Chronic Pelvic Pain
Nonspecific chronic pelvic pain (NSCPP) is a term used when persistent pelvic pain cannot be traced to a single, identifiable cause. For many people, this diagnosis can feel frustrating, but it’s more common than you might think. NSCPP often arises from a combination of factors, including changes in the central nervous system that make the body more sensitive to pain—a phenomenon known as central sensitization.
Pelvic floor dysfunction is another key contributor. When the pelvic floor muscles, which support the pelvic organs, become tense or uncoordinated, they can trigger ongoing discomfort. This dysfunction can develop after injury, surgery, or even prolonged stress. Psychological factors, such as anxiety, depression, or a history of trauma, can further amplify pain signals and make symptoms worse.
Treating nonspecific chronic pelvic pain requires a holistic, multidisciplinary approach. Pelvic floor physical therapy is a cornerstone of care, helping to relax and retrain the pelvic floor muscles through targeted exercises, myofascial physical therapy, and guided physical therapy evaluation. Addressing pelvic floor dysfunction can significantly reduce pain and improve function. In addition, therapies that support the central nervous system—such as mindfulness, counseling, and stress management—can help break the cycle of pain. By combining physical therapy with psychological support, many people with NSCPP find meaningful relief and a path forward.
Why “Just Relax” is Bad Advice
Daniel spent years hearing doctors say, “You just need to relax.” As he noted in his conversation with Adam at Pelvis NYC, this advice is often shame-based. If a man could simply choose to relax a muscle that has been clenched for seven years, he would. The problem is that the sympathetic nervous system (the fight-or-flight branch) has taken over. Persistent pain is a key feature of chronic pelvic pain, often resulting from central sensitization, which can increase the risk of heightened pain perception and complicate treatment.
The Brain-Bladder-Bowel Connection
The pelvic floor is unique because it reacts directly to emotional stress. This is why many men with pelvic pain also suffer from Bruxism (jaw clenching). Mental health conditions such as depression and anxiety are common among individuals with chronic pelvic pain and can worsen pain perception. The body is stuck in a “Global High Tone” state. Pelvic floor therapy is the “manual override” for this system.
Chronic Pelvic Pain Related Conditions
Chronic pelvic pain rarely exists in isolation—it’s often intertwined with other health conditions that affect the pelvic region. Some of the most common related conditions include endometriosis, pelvic inflammatory disease (PID), interstitial cystitis, and irritable bowel syndrome (IBS).
Endometriosis occurs when tissue similar to the lining of the uterus grows outside the uterus, causing inflammation, scarring, and significant pelvic pain. Pelvic inflammatory disease is an infection of the female reproductive organs that can lead to chronic discomfort if not treated promptly. Interstitial cystitis, also known as painful bladder syndrome, involves chronic inflammation of the bladder, resulting in pelvic pain and frequent urination. Irritable bowel syndrome is a digestive disorder that can cause abdominal pain, bloating, and changes in bowel habits, often overlapping with chronic pelvic pain.
Each of these conditions may require its own specific treatment—ranging from antibiotics for PID, hormonal therapy or surgery for endometriosis, to dietary changes and medications for IBS and interstitial cystitis. Recognizing and addressing these related conditions is essential for effectively managing chronic pelvic pain and improving overall well-being.
How Pelvic Floor Physical Therapy (PFPT) Works

Physical therapy for the pelvic floor is the gold standard for treating CPPS and post-surgical dysfunction. Unlike general physical therapy, which might focus on “reps” and “strengthening,” PFPT for hypertonicity focuses on down-training and release.
Management of chronic pelvic pain typically focuses on symptom relief and addressing both physical and psychological contributors.
Myofascial pain syndrome is a common muscular contributor to chronic pelvic pain and can be addressed through targeted physical therapy.
1. Nervous System Regulation
At Pelvis NYC, the treatment begins by making the patient feel safe. For someone like Daniel, who associated “people being in his body” with pain, this was crucial. By using trauma-informed care, therapists help the patient transition from a sympathetic (stressed) state to a parasympathetic (relaxed) state.
2. Manual Therapy and Biofeedback
Therapists use internal and external manual techniques to find “trigger points” in the pelvic floor. Assessment of pelvic floor tenderness and evaluation of the pelvic floor musculature are important components of physical therapy for chronic pelvic pain.
- External Work: Addressing the abdominals, glutes, and inner thighs, which often tighten in sympathy with the pelvic floor.
- Internal Work: Gentle pressure applied to the levator ani muscles to encourage them to let go.
- Biofeedback: Helping the patient “see” or feel the difference between a contracted muscle and a relaxed one.
3. Reframing the Narrative
A major part of Daniel’s breakthrough was the 3-month mark. He realized his progress wasn’t a fluke. By understanding the “why” behind his pain, he was able to stop viewing his body as an enemy.
Alternative Therapies for Chronic Pelvic Pain
For many people living with chronic pelvic pain, alternative therapies can offer valuable support alongside conventional medical treatments. Acupuncture, a practice rooted in traditional Chinese medicine, uses fine needles to stimulate specific points on the body and has been shown in some studies to provide pain relief for chronic pelvic conditions.
Cognitive-behavioral therapy (CBT) is another powerful tool, helping individuals manage the stress, anxiety, and depression that often accompany chronic pelvic pain. By learning new coping strategies and reframing negative thought patterns, patients can reduce the emotional impact of their symptoms.
Physical therapy—especially pelvic floor physical therapy—remains a cornerstone of alternative care, targeting pelvic floor dysfunction and promoting relaxation of the pelvic floor muscles. Other approaches, such as yoga, meditation, and massage, can further support pain relief and overall well-being. While these therapies can be highly beneficial, it’s important to work with your healthcare provider to ensure they complement your overall treatment plan and address your unique needs.
The Importance of Queer-Affirming Pelvic Care
A significant barrier for many men—especially in the queer community—is finding a provider who understands sexual health beyond just “reproduction.”
Daniel highlighted that many proctologists were dismissive of his desire to return to a healthy sex life as a gay man. Specialized care at Pelvis NYC provides:
- Judgment-free dialogue about anal sex and intimacy.
- Gender-affirming care that recognizes the specific needs of queer bodies.
- Anatomical expertise on how pelvic tension affects both bowel function and sexual pleasure.
Chronic Pelvic Pain Treated with Multidisciplinary Care
Successfully treating chronic pelvic pain often requires a team-based, multidisciplinary approach. Because CPP can stem from a variety of sources—muscular, neurological, gastrointestinal, or urological—a comprehensive treatment plan is essential. This plan may involve collaboration between gynecologists, urologists, gastroenterologists, pain management specialists, and physical therapists.
Physical therapy, particularly pelvic floor physical therapy, plays a central role in addressing pelvic floor dysfunction and restoring normal muscle function. For conditions like interstitial cystitis, treatment may also include medications, bladder training, and dietary modifications. Pain management specialists can offer additional strategies for pain relief, such as nerve blocks or nonsteroidal anti-inflammatory drugs, while psychologists or counselors can help address the emotional and psychological aspects of chronic pelvic pain.
By combining medical, physical, and psychological therapies, a multidisciplinary team can create an individualized treatment plan that targets all aspects of chronic pelvic pain. This holistic approach not only helps relieve pain but also improves health-related quality of life outcomes, empowering patients to reclaim their lives and move forward with confidence.
Comparison: Traditional Care vs. Pelvic NYC Holistic Approach
| Feature | Traditional Specialist (Proctologist/Urologist) | Pelvis NYC Holistic Approach |
| Focus | Structural damage (tears, lumps, infections) | Muscle function and nervous system tone |
| Primary Tool | Surgery or Medication (Antibiotics/Botox) | Manual therapy, breathing, and education |
| Bedside Manner | Often clinical and dismissive of “feelings” | Trauma-informed and patient-first |
| Sexual Health | Often ignored or told “it’s permanent” | Integrated as a primary goal of recovery |
| Outcome | Fixed the tear, but the pain remains | Restored function and eliminated the fear of pain |
FAQ: Common Questions About Male Pelvic Floor Therapy
Can pelvic floor therapy help after a failed surgery?
Yes. Many patients have “successful” surgeries (the fissure is healed) but still have “unsuccessful” outcomes (the pain is still there). PT addresses the muscular habits and nerve sensitivity that surgery cannot fix.
How long does it take to see results?
While every body is different, Daniel noticed a significant shift around the 3-month mark. Consistency is key to retraining the nervous system.
Is pelvic floor therapy only for people who have had surgery?
Not at all. It is highly effective for “unexplained” pelvic pain, frequent urination, erectile dysfunction, and constipation.
Do I have to do internal work?
Internal work is often the most effective way to reach the affected muscles, but it is always performed with consent and at the patient’s pace. It is a medical procedure, not a sexual one.
Conclusion: You Are Not Your Trauma
Daniel’s journey from being “in a diaper for six months” and feeling “broken” to living a life free of chronic pain is a testament to the power of specialized care. You don’t have to live in a loop of pain, tension, and fear.
The missing link in men’s healthcare isn’t a new pill or a more invasive surgery—it’s the understanding that the pelvic floor and the mind are inextricably linked.
Take the First Step Toward Healing
If you are struggling with pelvic pain, sexual dysfunction, or post-surgical complications, don’t wait years to seek help.
Book a Consultation with Pelvis NYC today. Our team specializes in helping men reclaim their bodies and their lives through expert, trauma-informed pelvic floor therapy.



No comment yet, add your voice below!